Prostate Cancer
With the American Cancer Society estimating that one in every six men will develop prostate cancer in their lifetime, it is the most common cancer among men. The good news is that prostate cancer is manageable and even curable in some cases with the proper treatment. For approximately 99 percent of men who have been diagnosed with prostate cancer, treatment has helped extend their lives by more than five years.
WHAT ARE THE MOST COMMON PROSTATE CANCER SYMPTOMS?
The prostate gland is located near the bladder and the urethra, which means that any abnormalities on the gland can produce urinary symptoms. Some warning signs to look out for include the following:
• Overall difficulty urinating, that is accompanied by burning or pain
• Loss of bladder control, or inability to control the flow of urine
• Blood in the urine
• Urges to urinate at night
If cancer has spread to other tissues or bones, other prostate cancer symptoms may arise, such as:
• Overall difficulty getting an erection
• Swelling or pain in the legs or pelvic area
• Painful ejaculation
• Blood in the semen
It’s important to keep in mind that these symptoms can be attributed to other conditions besides prostate cancer. Visit your doctor for an accurate diagnosis.
HOW IS PROSTATE CANCER TREATED?
If you or a family member has been diagnosed with prostate cancer, you should consult your physician. You will likely have a team of specialists, including a radiation oncologist, urologist, and a medical oncologist.
The types of therapy used to treat prostate cancer vary depending on each individual patient, with factors such as the stage of cancer and the patient’s personal health playing a key role in determining the treatment needed. Treatment methods include radiation therapy, surgery, chemotherapy, and more. Treatment methods may also be combined in some cases. For any questions about available prostate cancer treatments, ask your doctor for more information.
SpaceOAR™ FOR PROSTATE CANCER
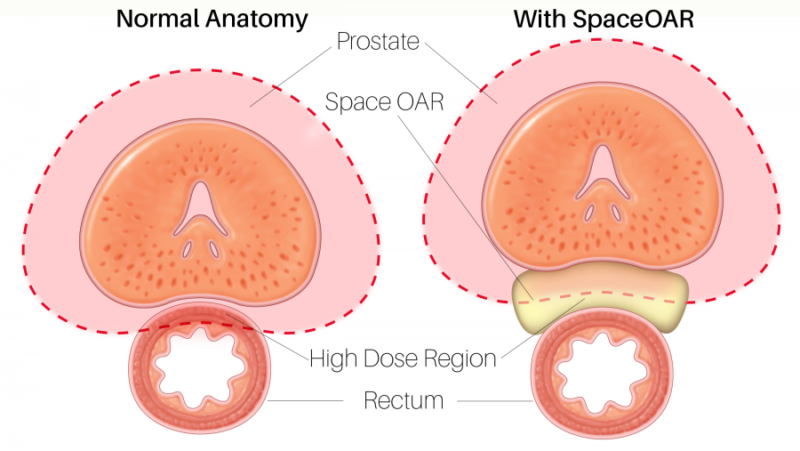
When treating prostate cancer patients with radiation therapy, the goal is to kill the cancer cells while avoiding damage to the surrounding healthy tissue. That’s why we have partnered up with SpaceOAR Hydrogel, a temporary injectable gel that provides space between the rectum and the prostate, making it much less likely that the rectum is exposed to radiation or damaged. By acting as a spacer, the hydrogel temporarily moves the rectum a half-inch (1.3 cm) away from the prostate.1 By separating the prostate from the rectum, SpaceOAR Hydrogel reduces the radiation dose delivered to the rectum and may eliminate or decrease damage.
RADIATION THERAPY FOR PROSTATE CANCER
Prostate cancer can be treated using radiation therapy, which utilizes focused rays of radiation on the target area to kill cancer cells while preserving healthy surrounding tissue. An advantage to radiation therapy compared to other treatment methods is organ-preservation, meaning that it minimizes the amount of healthy tissue affected by treatment.
External Beam Radiation Therapy (Radiotherapy)
This type of radiation therapy delivers targeted doses of radiation to treat prostate cancer, and in some cases, cure it. The process begins with a physical exam, and a CT scan to create a 3-D map that will serve as a guide for the beam. This ensures pinpoint accuracy during treatment. Sometimes your treatment plan will include not only the prostate but the seminal vesicles (glands on the back of the prostate) and lymph nodes. There are different methods for administering radiotherapy, so ask your doctor about what type you will be receiving during treatment.
This therapy is typically given in five-day sessions over the course of several weeks, but the actual frequency of your treatment can vary depending on your needs.
Brachytherapy
Brachytherapy is a treatment method that kills cancer cells internally by surgically inserting a small amount of radioactive material directly into the tumor. After treatment is complete, the material will be removed from the body. Brachytherapy is typically done as an outpatient procedure, meaning that you will be able to go home on the same day of the implant. The dosage and length of treatment vary on a case-by-case basis.
Brachytherapy may be combined with other forms of treatment, such as external beam radiation or hormone therapy, to possibly improve the cure rate.
HORMONE THERAPY
Hormone therapy can be used to treat prostate cancer by reducing testosterone production in the body. Lower levels of testosterone can shrink the tumor, and slow the progression of the cancer to the rest of the body. It’s common for hormone therapy to be combined with radiation therapy, usually done before and after the radiation treatment. The length of your hormone treatment depends on a variety of factors, including what other treatments you are currently undergoing, and the stage of your cancer. Your radiation oncologist, medical oncologist, or urologist may prescribe hormone therapy; be sure to ask your physician about any questions you may have.
POTENTIAL SIDE EFFECTS OF PROSTATE CANCER TREATMENT
Since external beam radiation therapy is noninvasive, side effects from treatment are rare. Brachytherapy, on the other hand, requires a small surgical procedure and does have some common side effects including swelling, soreness and frequent urination just after the procedure. However, these side effects are due to the surgical procedure, and not the radiation. If you are also receiving hormone therapy as part of your treatment, the possible side effects include hot flashes, mild breast tenderness, diarrhea, nausea and tiredness.
Many side effects that develop as a result of prostate cancer treatment can be controlled through medication and alterations to your normal diet, which your doctor can provide assistance with. Make sure to tell your doctor and nurse about any side effects you may be suffering from, so they can work to make you feel better and more comfortable.
PROSTATE CANCER RESOURCES
Malecare
212-844-8369
www.malecare.org
Prostate Cancer Foundation
1-800-757-CURE
www.prostatecancerfoundation.org
Us TOO! Prostate Cancer Education and Support
630-795-1002
www.ustoo.com
ZERO – Project to End Prostate Cancer
202-463-9455
www.zerocancer.org
Also see Helpful Links
BROCHURE
Download some helpful brochures from www.rtanswers.org
*Content provided by the American Society for Radiation Oncology, www.rtanswers.org, and the American Cancer Society.